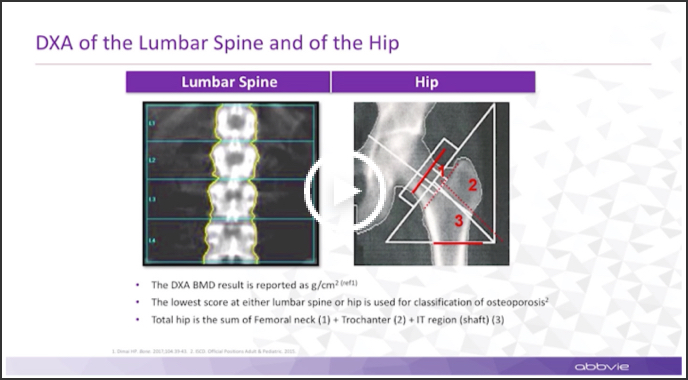
Hello. My name is Nelson Watts. I'm an endocrinologist by training but have been involved in osteoporosis research for quite a while. I'm currently Director of Osteoporosis and Bone Health Services for Mercy Health in Cincinnati and welcome you to this program on bone health sponsored by AbbVie. In this section, we'll begin with a review of basic bone physiology, examine strategies to identify patients at risk of bone loss, and clarify some of the effects of estrogen on bone. Bone is a dynamic tissue that provides structural and foundational support. It's made up of cortical bone on the outside and trabecular bone at the ends of the long bones and the centers of the vertebral bodies. Cortical, or compact bone, is the most prevalent in the skeleton, but the trabecular bone has a much greater surface area and is more metabolically active. Bone is renewed by a process called turnover, or remodeling.
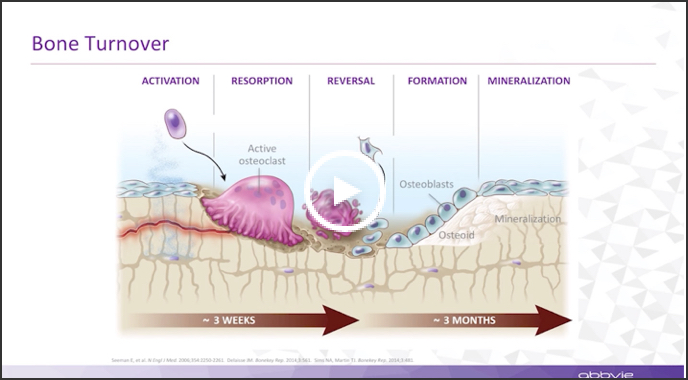
At any one time, there are millions of active bone remodeling sites in the body. Triggered by activation, bone-resorbing osteoclasts resorb a packet of bone. There's a brief reversal period where cleanup occurs. Then, bone-forming osteoblasts come in, producing the protein osteoid matrix that becomes mineralized and results in new bone. The entire remodeling process at a given site takes about three months. The goal would be to have balance—that is, the same amount of bone replaced as was removed. Much has been learned about how we can view this. The gold standard is a bone biopsy, but now we can get an idea of what's happening through chemical measurement of markers of bone resorption and markers of bone formation. From bone breakdown, we can measure end products of collagen degradation, C-telopeptide, or CTX, the carboxy terminal fragment of Type I collagen that is specific for bone, as well as the amino terminal fragment, NTx.
On the bone formation side, we can measure breakdown product of newly formed collagen, P1NP, procollagen type 1 in propeptide—that's the nitrogen N cleaved off of newly formed Type 1 collagen—enzymes, such as bone-specific alkaline phosphatase, or another protein breakdown product called osteocalcin. Bone turnover markers are of limited clinical utility. I have a talk on bone turnover markers with the subtitle, “not ready for prime time.” But markers do give us insights into dynamic changes and help us understand what happens with interventions.